Article
Feline OA is Real - How to Diagnose It Without Radiographs
Feline osteoarthritis (OA) is a widely under-recognized condition in clinical practice, particularly in India, where awareness about chronic pain in cats remains limited.
Epidemiological studies suggest that up to 61% of cats over the age of six show radiographic signs of OA, with the number rising significantly in cats over 12 years (Lascelles et al., 2012). However, due to the subtlety of feline behaviour and their evolutionary predisposition to mask pain, clinical detection is challenging.
Unlike dogs, cats with OA do not often exhibit overt lameness. Instead, veterinarians should look for reduced grooming, difficulty jumping onto furniture, reluctance to use the litter box, irritability, or social withdrawal. A validated owner questionnaire such as the Feline Musculoskeletal Pain Index (FMPI) or Client Specific Outcome Measures (CSOM) can
provide valuable insight into mobility changes that may not be obvious during examination (Benito et al., 2013).
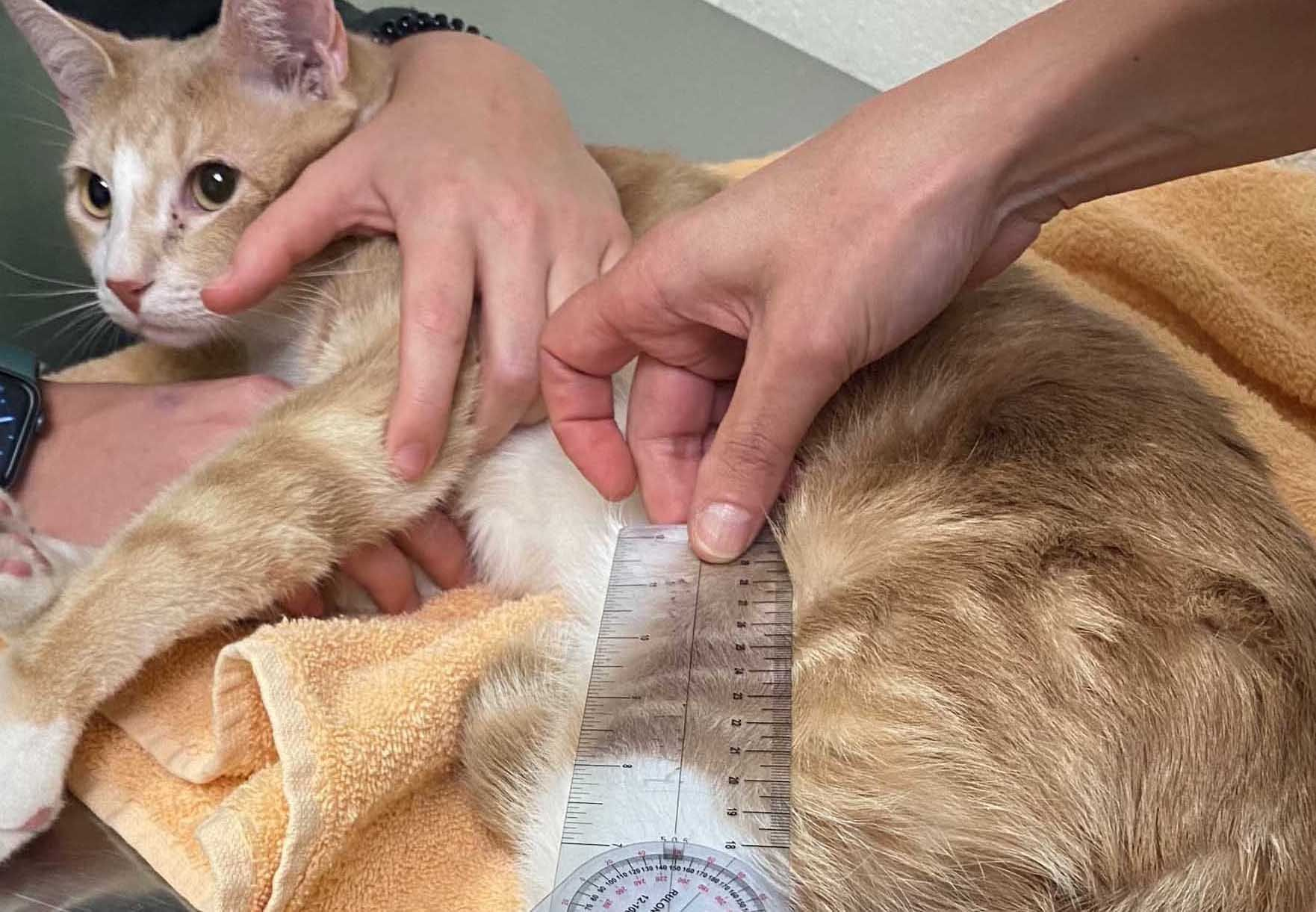
Orthopaedic examination in cats can be complicated by their temperament, but careful palpation of the spine, hips, elbows, and stifles may reveal crepitus, joint thickening, or reduced range of motion. Radiographs can confirm OA but often underestimate the pain burden; cats with mild radiographic changes may have significant functional impairment.
Management of feline OA should focus on pain control and environmental adaptation. Pharmacological options include meloxicam (off-label, at the lowest effective dose) and gabapentin, which provides analgesia and anxiolysis during handling. Non-drug approaches
include padded bedding, easy-access litter trays, warm resting spots, and ramps to reduce jumping. Newer therapies such as frunevetmab, a feline anti-NGF monoclonal antibody, show promise in clinical trials (Enomoto et al., 2022), though availability in India is still emerging.
Early recognition and a multimodal management strategy can greatly improve quality of life. Veterinary practitioners in India should prioritize feline OA in senior wellness exams, and educate guardians about behavioural pain signs.
References:
- Lascelles BDX et al. (2012). https://pubmed.ncbi.nlm.nih.gov/20561321
- Benito J et al. (2013). https://pubmed.ncbi.nlm.nih.gov/23369382
- Enomoto M et al. (2022). https://pubmed.ncbi.nlm.nih.gov/30368458
Related Contents

Article
Prognosis and Monitoring in Canine Leptospirosis: Knowing What to Expect
The clinical course of leptospirosis in dogs is highly variable, ranging from mild illness to fatal...

Article
Prevention and One Health Implications of Leptospirosis
Despite advances in diagnosis and treatment, leptospirosis continues to pose a significant threat du...

Article
Field Diagnosis of Newcastle Disease in Poultry
Newcastle Disease (ND) is a highly contagious viral infection of poultry that continues to cause sev...

Article
Vaccination Strategies Against Newcastle Disease – Field Perspectives
Vaccination remains the cornerstone of Newcastle Disease control in poultry production sys...

Article
Emerging Diagnostic and Vaccine Technologies in Newcastle Disease
Advances in molecular biology and vaccine technology are reshaping the approach to Newcastle Disease...

Article
Infectious Bursal Disease in Poultry: Understanding the Virus Beyond the Basics
Infectious Bursal Disease (IBD), commonly known as Gumboro disease, remains one...

Article
Pathogenesis and Clinical Expression of IBD: What Every Field Veterinarian Should Recognize Early
Infectious Bursal Disease is not just a viral infection, it is a disease of immune destruc...

Article
Diagnosis, Vaccination, and Field Control of IBD: Bridging Gaps Between Theory and Practice
Despite widespread vaccination, Infectious Bursal Disease continues to cause outbreaks globally. The...