Article
When Blood Pressure Turns Critical: Recognising Hypertensive Emergency in Small Animals
Arterial blood pressure in mammals is tightly regulated through neurohumoral, myogenic, metabolic, and flow-mediated mechanisms. However, systemic hypertension can develop secondary to various diseases in veterinary patients. In dogs, it is linked to conditions such as acute kidney injury (AKI), chronic kidney disease, diabetes mellitus, immune-mediated haemolytic anaemia, and pheochromocytoma. In cats, chronic kidney disease, hyperthyroidism, and primary hyperaldosteronism are the most common causes1.
Among hypertensive disorders, hypertensive emergency (HE) represents the most severe form, defined by marked elevation in blood pressure with concurrent target organ damage (TOD). Although veterinary thresholds are not standardised, the consequences, damage to the brain, eyes, kidneys, and heart, are well recognised 2.
Acute Clinical Presentation
Hypertensive emergency is typically acute in onset, with clinical signs often developing within a day. This rapid progression makes early recognition essential. In the study, seizures were the most common presenting complaint, emphasising the need to consider systemic hypertension in patients with acute neurological signs1.
Neurological abnormalities frequently included absent menace response, obtundation, anisocoria, and circling, consistent with hypertensive encephalopathy. Ocular findings were also prominent. Fundoscopic examination commonly revealed retinal detachment, followed by retinal haemorrhage. In patients presenting with acute blindness, retinal pathology was often confirmed, although distinguishing between ophthalmic and neurological causes remains important1.
The coexistence of neurological and ocular abnormalities should strongly raise suspicion for hypertensive emergency, particularly in patients with underlying systemic disease.
Target Organ Damage and Pathophysiology
Target organ damage is the defining feature of a hypertensive emergency. In veterinary patients, the most commonly affected organs include the brain, eyes, kidneys, and heart. Among these, neurological and ocular signs are the most clinically apparent2.
Hypertensive encephalopathy results from failure of cerebral autoregulation. The Baylis effect describes vasoconstriction in response to increased pressure, leading to reduced cerebral blood flow and ischaemic injury. In contrast, the “breakthrough theory” suggests that excessive pressure overwhelms autoregulation, resulting in vasodilation, vascular injury, and disruption of the blood–brain barrier. Both mechanisms ultimately lead to vasogenic oedema, a consistent finding in affected patients3.
Blood Pressure Measurement
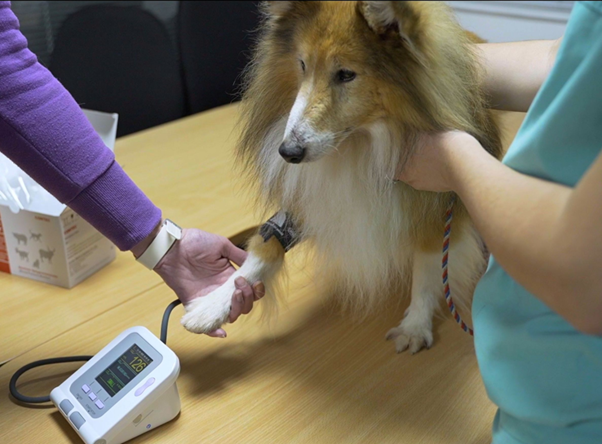
Accurate blood pressure measurement is critical for diagnosis. In this study, all cases were assessed using non-invasive Doppler techniques, following ACVIM guidelines. However, these methods have limitations, and results should be interpreted cautiously as no device fully meets validation standards1,2.
Although invasive arterial blood pressure (IBP) monitoring is the gold standard, it was rarely used, likely due to technical challenges and perceived risks such as infection or haemorrhage. Evidence suggests these risks are generally low1, and IBP should be considered more frequently in critical patients.
The degree of hypertension observed was severe, with dogs showing a median admission SBP of 220 mmHg and cats 230 mmHg, with peaks reaching 300 mmHg.
Diagnostic Workup and Underlying Causes
Identifying the underlying cause is essential for management. Laboratory findings frequently revealed renal dysfunction, with elevated creatinine levels particularly in non-survivors, highlighting the link between hypertension and kidney injury.
AKI was the most common underlying diagnosis in both species. In cats, causes included acute-on-chronic kidney disease, ureteral obstruction, and renal carcinoma. In dogs, AKI was associated with leptospirosis, suspected intoxication, and immune-mediated glomerulonephritis. Other causes included idiopathic hypertension and neoplasia1.
Clinical Relevance
Hypertensive emergency is a true veterinary emergency requiring rapid recognition and intervention. Blood pressure measurement should be routine in patients presenting with seizures, acute blindness, or altered mentation. Neurological and fundoscopic examinations are essential for identifying target organ damage.
In the absence of clear veterinary guidelines, clinicians must rely on clinical judgement and individual patient response. Early detection and timely intervention remain key to improving outcomes in these critically ill patients.
Reference
- Beeston D, Jepson R, Cortellini S. Evaluation of presentation, treatment and outcome in hypertensive emergency in dogs and cats: 15 cases (2003‐2019). Journal of Small Animal Practice. 2022 Oct;63(10):784-91. https://onlinelibrary.wiley.com/doi/pdfdirect/10.1111/jsap.13530
- Acierno MJ, Brown S, Coleman AE, Jepson RE, Papich M, Stepien RL, Syme HM. ACVIM consensus statement: guidelines for the identification, evaluation, and management of systemic hypertension in dogs and cats. Journal of veterinary internal medicine. 2018 Nov;32(6):1803-22. https://academic.oup.com/jvim/article-pdf/32/6/1803/66838718/jvim15331.pdf
- Church ME, Turek BJ, Durham AC. Neuropathology of spontaneous hypertensive encephalopathy in cats. Veterinary pathology. 2019 Sep;56(5):778-82. https://journals.sagepub.com/doi/pdf/10.1177/0300985819849500
Related Contents

Article
Prognosis and Monitoring in Canine Leptospirosis: Knowing What to Expect
The clinical course of leptospirosis in dogs is highly variable, ranging from mild illness to fatal...

Article
Prevention and One Health Implications of Leptospirosis
Despite advances in diagnosis and treatment, leptospirosis continues to pose a significant threat du...

Article
Field Diagnosis of Newcastle Disease in Poultry
Newcastle Disease (ND) is a highly contagious viral infection of poultry that continues to cause sev...

Article
Vaccination Strategies Against Newcastle Disease – Field Perspectives
Vaccination remains the cornerstone of Newcastle Disease control in poultry production sys...

Article
Emerging Diagnostic and Vaccine Technologies in Newcastle Disease
Advances in molecular biology and vaccine technology are reshaping the approach to Newcastle Disease...

Article
Infectious Bursal Disease in Poultry: Understanding the Virus Beyond the Basics
Infectious Bursal Disease (IBD), commonly known as Gumboro disease, remains one...

Article
Pathogenesis and Clinical Expression of IBD: What Every Field Veterinarian Should Recognize Early
Infectious Bursal Disease is not just a viral infection, it is a disease of immune destruc...

Article
Diagnosis, Vaccination, and Field Control of IBD: Bridging Gaps Between Theory and Practice
Despite widespread vaccination, Infectious Bursal Disease continues to cause outbreaks globally. The...