Article
Fundamentals of Blood Pressure Regulation in Dogs & Cats
Blood pressure regulation in dogs and cats is a dynamic process that ensures adequate tissue perfusion while maintaining vascular stability. In veterinary practice, however, blood pressure is often not routinely assessed until complications arise. Given that hypertension is a major contributor to cardiovascular and systemic disease, understanding its physiological basis is essential for effective clinical management.
Basic Principles of Blood Pressure
Blood pressure is the force exerted by circulating blood on the walls of blood vessels. It is determined by two primary factors: cardiac output and peripheral vascular resistance. Systolic pressure is generated during cardiac contraction, while diastolic pressure reflects the residual force during cardiac relaxation1,2.
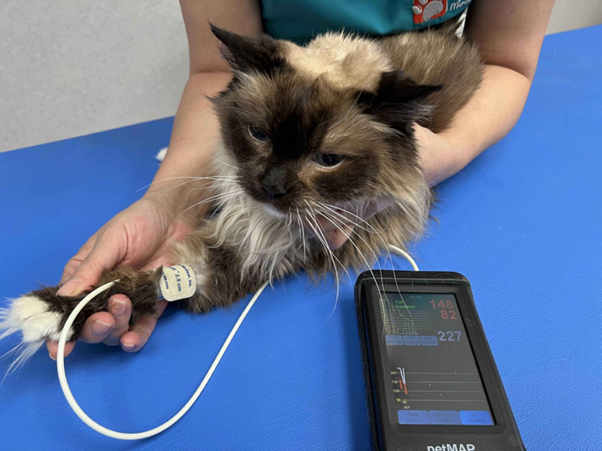
In dogs and cats, systolic blood pressure typically ranges from 120 to 130 mmHg, although readings may rise to 160 mmHg in clinical settings due to stress, commonly referred to as the white coat effect3. Persistent elevations beyond 140/90 mmHg are considered hypertensive and are associated with increased risk of organ damage1.
Cardiovascular Control Mechanisms
Blood pressure is directly influenced by the volume of blood pumped by the heart and the resistance offered by blood vessels. Increased cardiac output or vasoconstriction leads to elevated blood pressure. Conversely, vasodilation or reduced cardiac output lowers it.
The vasculature actively regulates this balance. Large arteries buffer pulsatile flow, while smaller arterioles control resistance. Structural changes such as vascular stiffening or narrowing contribute to sustained hypertension1.
Vasoactive Mediators in Regulation
A critical component of blood pressure regulation is the balance between vasodilatory and vasoconstrictive substances.
Nitric oxide (NO) is a key vasodilator that promotes vascular relaxation and reduces sympathetic activity. Reduced NO availability has been linked to hypertension, particularly under stress conditions1.
Bradykinin supports vasodilation and facilitates sodium excretion via renal mechanisms. Its effects are partly mediated through prostaglandin release, and impairment of this pathway may contribute to elevated blood pressure1.
In contrast, endothelin-1 (ET-1) is a potent vasoconstrictor. Increased production leads to vascular remodeling, oxidative stress, and persistent hypertension1.
Renin-Angiotensin-Aldosterone System (RAAS)
The RAAS is central to long-term blood pressure control. Angiotensin II induces vasoconstriction and stimulates aldosterone secretion, while also promoting vascular remodeling and fibrosis1.
Aldosterone increases sodium and water reabsorption in the kidneys, expanding blood volume and sustaining elevated blood pressure1. Persistent activation of this system is a key driver of chronic hypertension.
Renal Regulation
The kidneys play a crucial role in maintaining blood pressure by regulating fluid and electrolyte balance. When renal perfusion decreases, compensatory mechanisms promote sodium and water retention, increasing blood volume.
Chronic kidney disease is one of the most common causes of hypertension in dogs and cats. Impaired renal function disrupts normal regulatory pathways, leading to sustained elevation in blood pressure1.
Clinical Relevance for Veterinarians
In small animal practice, hypertension is most often secondary to underlying disease, rather than primary. Conditions such as renal disease and endocrine disorders frequently drive blood pressure elevation.
A major challenge is that hypertension often remains clinically silent until complications such as retinal damage, renal dysfunction, or cardiac changes occur. This highlights the importance of routine monitoring, particularly in at-risk populations.
Therapeutic strategies are closely linked to these physiological mechanisms. ACE inhibitors target RAAS activity, calcium channel blockers reduce vascular resistance, and vasodilators improve blood flow. Effective treatment depends on understanding the underlying disturbance.
Conclusion
Blood pressure regulation in dogs and cats involves a complex interaction between cardiac function, vascular tone, renal control, and hormonal signaling. Disruption of these mechanisms leads to hypertension, which has significant clinical implications.
For veterinarians, integrating routine blood pressure assessment with a strong understanding of underlying physiology allows for earlier diagnosis, targeted therapy, and improved patient outcomes.
Reference
- Adejumobi OA, Jeremiah OT, Omobowale TO. Blood pressure regulation and mechanism of hypertension development in dogs and cats: A review. Journal of Animal Science and Veterinary Medicine. 2022 Jun;7(3):103-12. https://www.academia.edu/download/99881610/342C36656.pdf
- Lombardi C, Pengo MF, Parati G. Systemic hypertension in obstructive sleep apnea. Journal of thoracic disease. 2018 Dec;10(Suppl 34):S4231. https://pmc.ncbi.nlm.nih.gov/articles/PMC6321893/pdf/jtd-10-S34-S4231.pdf
- Fang S, Livergood MC, Nakagawa P, Wu J, Sigmund CD. Role of the peroxisome proliferator activated receptors in hypertension. Circulation research. 2021 Apr 2;128(7):1021-39. https://www.ahajournals.org/doi/pdf/10.1161/CIRCRESAHA.120.318062
Related Contents

Article
Prognosis and Monitoring in Canine Leptospirosis: Knowing What to Expect
The clinical course of leptospirosis in dogs is highly variable, ranging from mild illness to fatal...

Article
Prevention and One Health Implications of Leptospirosis
Despite advances in diagnosis and treatment, leptospirosis continues to pose a significant threat du...

Article
Field Diagnosis of Newcastle Disease in Poultry
Newcastle Disease (ND) is a highly contagious viral infection of poultry that continues to cause sev...

Article
Vaccination Strategies Against Newcastle Disease – Field Perspectives
Vaccination remains the cornerstone of Newcastle Disease control in poultry production sys...

Article
Emerging Diagnostic and Vaccine Technologies in Newcastle Disease
Advances in molecular biology and vaccine technology are reshaping the approach to Newcastle Disease...

Article
Infectious Bursal Disease in Poultry: Understanding the Virus Beyond the Basics
Infectious Bursal Disease (IBD), commonly known as Gumboro disease, remains one...

Article
Pathogenesis and Clinical Expression of IBD: What Every Field Veterinarian Should Recognize Early
Infectious Bursal Disease is not just a viral infection, it is a disease of immune destruc...

Article
Diagnosis, Vaccination, and Field Control of IBD: Bridging Gaps Between Theory and Practice
Despite widespread vaccination, Infectious Bursal Disease continues to cause outbreaks globally. The...