Article
A Clinical Case of Feline Dermatophytosis Managed with Combined Antifungal Therapy
Dermatological disorders in companion animals may arise from multiple causes, including parasitic, bacterial, fungal, allergic, immunologic, nutritional, endocrine, and neoplastic conditions1. Among fungal infections, dermatophytosis is one of the most commonly encountered in dogs and cats and is recognized for its contagious and zoonotic potential, although it is typically non-life-threatening and treatable2.
Dermatophytes are classified as anthropophilic, geophilic, or zoophilic based on their habitat3. The most frequently reported agents include Microsporum canis, Microsporum gypseum, and Trichophyton mentagrophytes, with M. canis being the most common in companion animals1.
Clinical Presentation
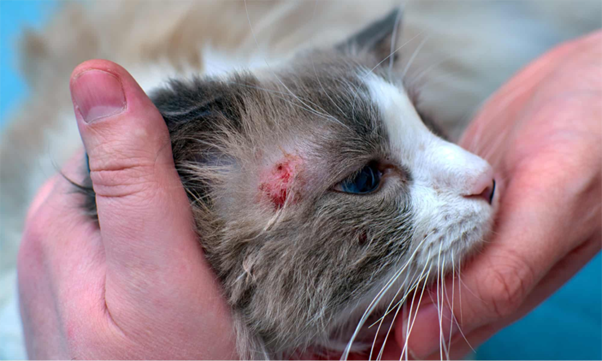
A 2-year-old male Persian cat weighing approximately 2 kg was presented with dermatological complaints suggestive of dermatophytosis.
On examination, patchy alopecia was observed over the head and ears, along with scaling, crusting, and signs of pruritus. Such lesions are consistent with commonly described dermatophytic presentations, particularly involving the head region1.
Initial Diagnostic Evaluation
A Wood’s lamp examination revealed green fluorescence on the affected hair shafts. While this finding may be suggestive of Microsporum canis, it is not specific and may also result from external contaminants or other materials1. Therefore, it was considered a screening tool only.
Direct microscopic examination using 10% potassium hydroxide (KOH) preparation did not demonstrate fungal elements4. However, given the limited sensitivity of this method, false-negative results were considered possible.
Routine hematological parameters were within normal limits, with no evidence of systemic involvement.
Confirmatory Diagnosis
Skin scrapings were cultured on Sabouraud dextrose agar and incubated at room temperature. After 7 days, fungal growth was observed.
The colonies appeared flat, white to cream in color, with a powdery to granular surface—features consistent with Trichophyton mentagrophytes1.
Microscopic examination using lactophenol cotton blue staining revealed macroconidia, supporting the presumptive identification of T. mentagrophytes. Although additional confirmatory tests such as urease activity were not performed, the morphological findings were considered sufficiently indicative1.
Fungal culture was regarded as the most reliable diagnostic method in this case.
Treatment Approach
Based on clinical and mycological findings, a combined therapeutic approach was initiated.
The cat was treated with oral itraconazole at approximately 10 mg/kg once daily for 20 days, along with topical ketoconazole applied twice daily for 35 days1.
Combination therapy was selected because topical treatment alone may not adequately penetrate hair follicles. Systemic antifungal therapy is often required for effective management of infections involving hair shafts1.
Clinical Outcome
Gradual clinical improvement was observed during the treatment period, including reduction in scaling, crusting, and pruritus, along with progressive hair regrowth.
Complete resolution of lesions was achieved after approximately 42 days of therapy. Continued treatment beyond apparent clinical cure is generally recommended until negative fungal cultures are obtained, in order to reduce the risk of recurrence.
Clinical Insights
This case highlights that clinical signs of dermatophytosis may be variable and overlap with other dermatological conditions, making diagnosis based on appearance alone unreliable .
Screening tools such as Wood’s lamp examination and KOH microscopy may provide supportive information but should be interpreted cautiously due to the possibility of false-positive and false-negative results.
Fungal culture remains the gold standard for definitive diagnosis.
Conclusion
This case demonstrates that a structured diagnostic approach, supported by fungal culture, can aid in accurate diagnosis of dermatophytosis in cats.
The use of combined systemic and topical antifungal therapy, along with appropriate treatment duration, may result in favorable clinical outcomes. Careful follow-up is advisable to ensure complete resolution and to minimize the risk of recurrence and zoonotic transmission.
References
- Indarjulianto S, Yanuartono Y, Nururrozi A, Raharjo S, Ajiguna JC. Combination of systemic and topical treatment for feline dermatophytosis: A case report. Acta Veterinaria Indonesiana. 2020 Jan 31;8(1):18-23. https://www.researchgate.net/profile/Yanuartono-Kaswarjono/publication/339535090_Combination_of_Systemic_and_Topical_Treatment_for_Feline_Dermatophytosis_A_Case_Report/links/5e7115a392851c93e0aa2662/Combination-of-Systemic-and-Topical-Treatment-for-Feline-Dermatophytosis-A-Case-Report.pdf
- Jackson EP. Analysis of dermatophyte prevalence and associated risk factors in rabbits (Master's thesis, Universidade de Lisboa (Portugal)). https://repositorio.ulisboa.pt/bitstreams/b2642ea1-edc0-4c83-80f5-ad2fe1672a8d/download
- Moskaluk AE, VandeWoude S. Current topics in dermatophyte classification and clinical diagnosis. Pathogens. 2022 Aug 23;11(9):957. https://www.mdpi.com/2076-0817/11/9/957
- Priyadharshini KS, Rajesh S, Divya B, Nirmala S. 10% Potassium Hydroxide Mount of Skin Scraping-A Simple Tool for Diagnosing Dermatophytosis in Patients Attending a Dermatology Clinic in a Tertiary Care Hospital in Salem. Journal of Health and Technology. 2025 Jun 25:106-14. https://ejournal-tnmgrmu.ac.in/index.php/health/article/download/83/58
Related Contents

Article
Prognosis and Monitoring in Canine Leptospirosis: Knowing What to Expect
The clinical course of leptospirosis in dogs is highly variable, ranging from mild illness to fatal...

Article
Prevention and One Health Implications of Leptospirosis
Despite advances in diagnosis and treatment, leptospirosis continues to pose a significant threat du...

Article
Field Diagnosis of Newcastle Disease in Poultry
Newcastle Disease (ND) is a highly contagious viral infection of poultry that continues to cause sev...

Article
Vaccination Strategies Against Newcastle Disease – Field Perspectives
Vaccination remains the cornerstone of Newcastle Disease control in poultry production sys...

Article
Emerging Diagnostic and Vaccine Technologies in Newcastle Disease
Advances in molecular biology and vaccine technology are reshaping the approach to Newcastle Disease...

Article
Infectious Bursal Disease in Poultry: Understanding the Virus Beyond the Basics
Infectious Bursal Disease (IBD), commonly known as Gumboro disease, remains one...

Article
Pathogenesis and Clinical Expression of IBD: What Every Field Veterinarian Should Recognize Early
Infectious Bursal Disease is not just a viral infection, it is a disease of immune destruc...

Article
Diagnosis, Vaccination, and Field Control of IBD: Bridging Gaps Between Theory and Practice
Despite widespread vaccination, Infectious Bursal Disease continues to cause outbreaks globally. The...