Article
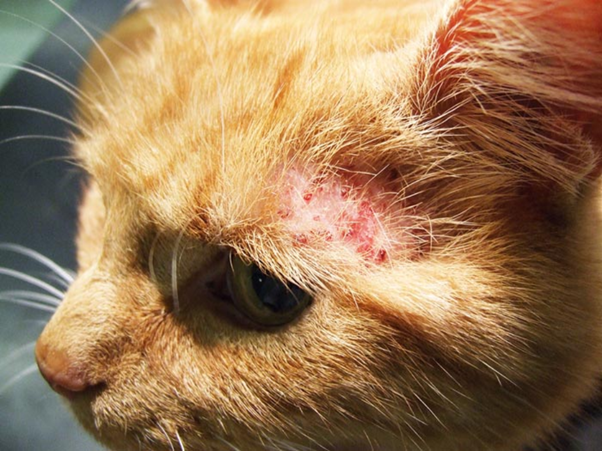
Feline Allergic Dermatitis — A Practical, Stepwise Diagnostic Approach
Once the complexity of feline allergic dermatitis is understood, the solution lies in discipline. The 2023 AAHA guidelines emphasize that successful diagnosis depends on a structured, stepwise approach—not clinical intuition1.
Step 1: Rule Out Ectoparasites First
Fleas remain the most common cause of allergic dermatitis in cats, and indoor status does not eliminate risk. The absence of visible fleas does not rule out flea allergy, making empirical treatment a practical necessity in many cases. Treating all in-contact animals is equally important to prevent reinfestation1.
Step 2: Perform the Minimum Dermatologic Database
A minimum dermatologic database (MDB) is essential and should include skin cytology, ear cytology, skin scrapings, and dermatophyte testing. Dermatophytosis is particularly important in cats, as it can closely mimic allergic disease. Skipping this step risks missing treatable conditions and delays accurate diagnosis.
Step 3: Control Secondary Infections
Secondary infections, including bacterial and Malassezia dermatitis, must be addressed early. These infections can significantly increase pruritus, mask the underlying disease, and reduce the effectiveness of antipruritic therapies. Treating them is not optional—it is foundational.
Step 4: Conduct a Diet Trial
A diet trial remains the only reliable method to diagnose food allergy. No clinical signs can distinguish food allergy from atopy, making this step essential. The protocol requires strict dietary exclusion for 4–12 weeks, followed by rechallenge to confirm diagnosis. In cats, compliance challenges—such as food selectivity and multi-pet households—often complicate execution, but this does not diminish its importance1.
Feline Atopy — A Diagnosis of Exclusion
Once ectoparasites and food allergy have been ruled out, feline atopic dermatitis can be diagnosed. Allergy testing should not be used to diagnose atopy; its role is limited to identifying allergens for immunotherapy. Misuse of these tests remains a common clinical error1.
Treatment Considerations — Cats Are Different
Treatment strategies in cats differ significantly from dogs. Glucocorticoids are often highly effective and commonly used as first-line therapy. Cyclosporine is well-supported for long-term management. While oclacitinib and lokivetmab are widely used in dogs, their use in cats is off-label, with limited but emerging evidence. Clinical judgment is essential when adapting these therapies.
Practical Clinical Strategy
Managing pruritic cats effectively requires consistency. Each case should begin with flea control, followed by a minimum dermatologic database. Secondary infections must be treated promptly, and a diet trial should be initiated where indicated. Only after these steps are completed should atopy be considered.
Final Takeaway
Feline allergic dermatitis is not solved through shortcuts—it is solved through process. In cats, diagnosis is not about recognition—it is about exclusion done right.
Reference
- Miller J, Simpson A, Bloom P, Diesel A, Friedeck A, Paterson T, Wisecup M, Yu CM. 2023 AAHA management of allergic skin diseases in dogs and cats guidelines. Journal of the American Animal Hospital Association. 2023 Nov 1;59(6):255-84. https://www.aaha.org/wp-content/uploads/globalassets/02-guidelines/2023-aaha-management-of-allergic-skin-diseases-in-dogs-and-cats-guidelines/resources/2023-aaha-management-of-allergic-skin-diseases-guidelines.pdf
Related Contents
Article
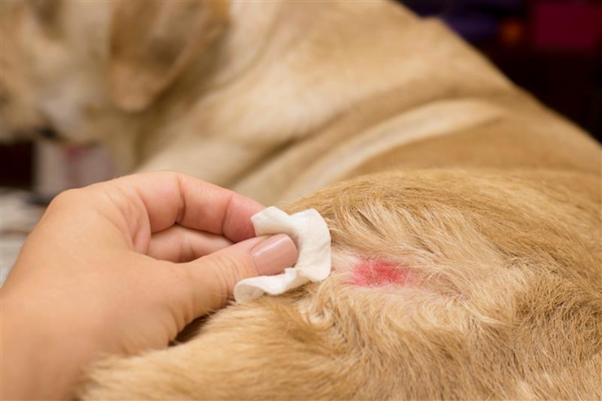
The Diagnostic Discipline of Pruritus – Why Structure Beats Guesswork
Pruritus remains one of the most common presenting complaints in small animal practice, ye...
Article
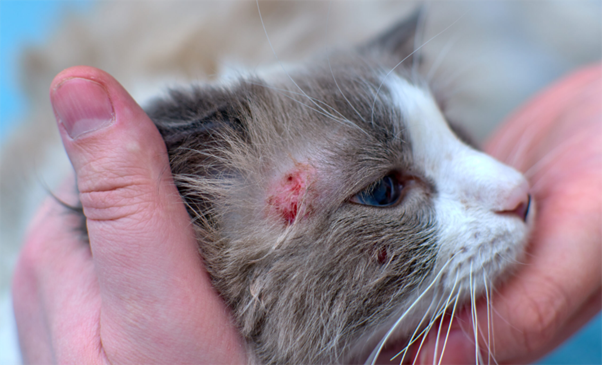
Feline Allergic Dermatitis — Why Diagnosis is So Challenging
Feline allergic dermatitis does not follow predictable rules—and that is exactly why it is so...

Article
Food Allergies in Cats – Managing the Fussy Eaters
Food allergies are a common, yet often under-recognized cause of chronic pruritus in cats. Unlike do...
.jpg)
Article
Feline Atopic Skin Syndrome (FASS) – Beyond the Itch
Feline Atopic Skin Syndrome (FASS) is a chronic, inflammatory skin condition triggered by...
Article
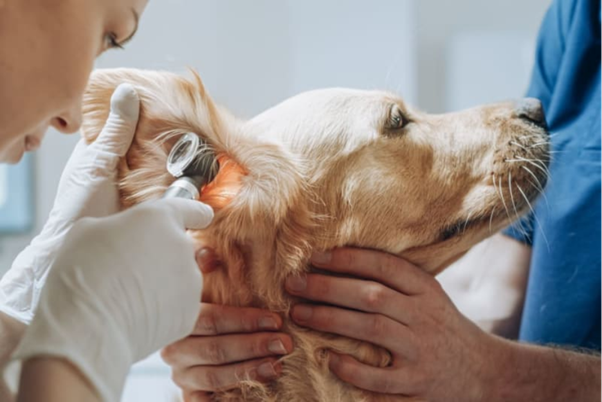
Allergic Otitis Externa in Dogs and Cats: Diagnosis and Management
Allergic otitis externa (AOE) is a frequent manifestation of allergy in companion animals...

Article
Spectrum of Care Considerations in Managing Allergic Skin Diseases
Allergic skin diseases are among the most common medical conditions in dogs and cats, with skin alle...
Article
Uterine Biopsy in the Subfertile Bitch: Moving from Theory to Clinical Decision-Making
Endometrial biopsy has long been a cornerstone in evaluating reproductive health in large animals, p...

Article
Understanding Uterine Lesions in Canine Subfertility: What Really Matters Clinically?
Subfertility in the bitch is a multifactorial problem, often frustrating for both clinicians and bre...